Infectious Disease & Airway Management
Preparing the Emergency Room for the Next Pandemic
Breathing problems were commonly experienced by patients who contracted COVID-19. Many who became sick with the virus were unable to oxygenate themselves adequately. In response to this issue, many doctors in hospitals found themselves performing intubations. Intubation is a procedure that places a tube in the airway of a patient to put a patient on mechanical ventilation. Due to the way COVID is transmitted, this often places healthcare workers in the direct line of fire of contracting coronavirus from the patient's airway.
For David Wright, MD, chair of the Department of Emergency Medicine at Emory, his biggest concern when the pandemic began to unfold was "the exposure of my staff in the most incredibly high-risk scenarios. Everybody coming in was a potential COVID patient at that time and we were unclear how protected we were, especially in an invasive procedure like intubation where aerosolization occurs," said Wright. He then reached out to his brilliant friends, Russell Gore, MD and Adam Klein, to put their heads together and find a way to protect clinical faculty during these life-saving procedures.

David Wright
Gore is a clinical neurologist practicing at the Shepherd Center and conducting research through GA Tech and Emory. Gore and Wright worked together on many innovation projects over the years, and Gore's 8-year career in the military made him accustomed to practical innovation projects involving austere environments. "When David and I spoke, it resonated with the that this was a real threat and risk. If we start losing emergency medicine staff members, what is that going to mean for our healthcare system moving forward? We put our heads together to very quickly try to come up with a solution to protect emergency medicine providers," Gore explained.
Adam Klein, MD, is the Chief of the Division of Laryngology and the Director of the Emory Voice Center. In the Emory Voice Center, they spend a lot of time in the throat and the airways. "Just like anesthesiologists and Wright's team, we are spending a lot of time in an area that is very high risk during COVID," said Klein, "When Russell gave me a call and said he had been working with David, it clicked immediately that we all had the same concerns and were facing the same threats."

Adam Klein
"When we first began in March, we needed something quick," Wright explained, "We created some of the earlier devices that were not perfect, and we knew they were not perfect. This helped us with our new design, which is a design for the future."
Using their combined skills to address their shared concerns, this team came up with the Infection Control System for Resuscitation and Airway Management. This device is essentially a pop-tent that can be easily deployed and stored. This tent is placed over the patient and has two core elements: it has splatter and aerosol protection, and it allows for adequate patient access that does not get in the way of the care of the patient.
In a clinical setting, infectious threat precautions are typically separated into contact and aerosolized precautions. Contact precautions are something that may be transmitted via body fluid splattering and saliva. Aerosolized pathogens are tiny particles that float in the air and then make contact with another individual through inhaling in or through contact with the eyes or other mucus membranes.
A lot of the initial solutions to this pandemic and clinical precautions thought about contact precautions, and very few efforts were focused on aerosolized particles. "Everyone was much more worried about handwashing and surfaces than about the air that we share with others. We were worried about aerosol precautions quite early as compared to a lot of other folks. That is what led to this device," said Gore.
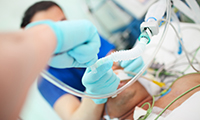
Intubation
The current design of this device provides coverage for all the staff that may be exposed during intubation, including those at the foot of the bed. This sets this device apart from other devices created for protection, as it addresses exposure beyond just the head of the hospital bed.
"Controlling aerosolized viruses is challenging," Klein explained, "We wanted to design something more than a glorified shield, we wanted to make sure the aerosolized particles were contained within our version of this intubation tent."
With this design, the research team created an enclosure that protects the space that healthcare workers are operating in. "That is something that a lot of folks do not think about," Gore explained, "You want to protect the individual, but in a busy medical environment you have to be able to manage a patient quickly and turn that space over to manage the next patient. A contaminated environment takes a lot of resources to decontaminate and keep up with the clinical tempo and the volume that may be coming in an emergency."
"As we moved towards the design that we have now, another element that sets us apart is that we wanted a design that is easy to store," said Gore, "Our expectation is that everyone will want to be more prepared for the next pandemic than we were for this one, we wanted a device that has a long shelf-life, is easy to store, easy to deploy, and is disposable."
“The technology that our researchers have developed is truly outstanding, and will help emergency rooms become a safer place for everyone,” said Raj Guddneppanavar, Assistant Director, Licensing at Emory OTT.
The device is not currently deployed in healthcare settings and is currently in the prototyping phase. The team has received a grant from the Georgia Research Alliance that has allowed them to optimize the design and troubleshoot some of the metrics. Soon they plan to gather more information by deploying it in various healthcare settings and getting feedback from providers. Their goal is that this device will be stored in healthcare settings in preparation for any future emergencies and pandemics.
Techid: 20137
Read our technology brief